Prostate Cancer
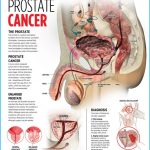
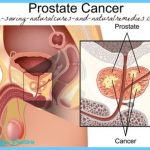
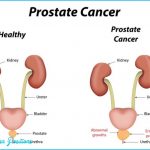
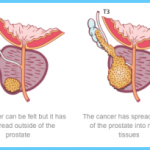
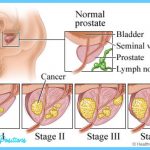
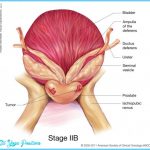
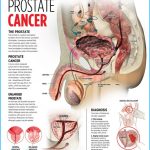
The prostate gland is situated at the base of the bladder in men; if enlarged, it can block the flow of urine. Prostate cancer is the most common cancer in men and the second leading cause of cancer death in men. Nearly 259,000 new cases of prostate cancer are diagnosed and nearly 30,000 American men die from the disease each year.
Age is the strongest predictor of the risk of prostate cancer, with about 62% of cases diagnosed in men over age 65, and 97% of cases occurring in men over age 50. Inherited genetic predisposition may be responsible for 5-10% of cases; men with a family history of the disease should be vigilant about screening. Diets high in calories, dairy products, refined grains, and animal fats and low in plant foods have been implicated as possible culprits, as have obesity, inactivity, and a history of sexually transmitted diseases. Type 2 diabetes and insulin resistance are also associated with prostate cancer. Diet may be an important means of preventing prostate cancer. Soy foods, tomatoes, and cruciferous vegetables are being investigated for their possible protective effects.
Some cases are first detected by rectal examination during a routine physical exam. During this exam, a physician feels the prostate through the rectum to determine if the gland is enlarged or if lumps are present. Ultrasound and biopsy may also be used to detect and diagnose prostate cancer. A specialized test, called the prostate-specific antigen (PSA) blood test, is commonly used to detect prostate cancer and can be useful, but the test is controversial because it can yield false-positive results. The ACS recommends that men be given information about the benefits and limitations of the tests. Both the rectal exam and the PSA test should be offered annually, beginning at age 50 for men at average risk and at age 45 for men at high risk, including African Americans and those with a family history of the disease.
Prostate Cancer Photo Gallery
Beginning in their twenties, women should be told about the benefits and limitations of BSE. Women should be aware of how their breasts normally look and feel and report any new breast changes to a health professional as soon as they are found. Finding a breast change does not necessarily mean there is a cancer.
A woman can notice changes by knowing how her breasts normally look and feel and by feeling her breasts for changes (breast awareness), or she can choose to use a step-by-step approach and use a specific schedule to examine her breasts.
Women with breast implants can do BSE. It may be useful to have the surgeon help identify the edges of the implant so that you know what you are feeling. There is some thought that the implants push out the breast tissue and may make it easier to examine. Women who are pregnant or breast-feeding can also choose to examine their breasts regularly.
If you choose to do BSE, the following information provides a step-by-step approach for the exam. The best time for a woman to examine her breasts is when the breasts are not tender or swollen. Women who examine their breasts should have their technique reviewed during their periodic health exams by their health care professional.
It is acceptable for women to choose not to do BSE or to do BSE occasionally. Women who choose not to do BSE should still know how their breasts normally look and feel and report any changes to their doctor right away.