It’s well documented that hyperthyroidism causes a higher rate of bone breakdown. In fact, the latest research shows that even low-level Graves’ disease is associated with bone turnover. A study soon to be published in the Annals of Internal Medicine (in press at the time of writing this blog) revealed that among 9400 older women, those with low-grade hyperthyroidism had a three-fold greater risk of hip and vertebral fractures.7
Some studies have found a harmful effect of anti-thyroid medication on bone density. To explore further the effect of thyroid medication on bone loss, French researchers summarized the results from 41 studies in 1250 patients.8 Their results
showed that medications like Tapazole® (methimazole) and Propyl-Thyracil® (propylthiouracil) that suppress thyroid hormone secretion cause significant bone loss in the lower spine and hip in postmenopausal women.
There is also evidence that women with Graves’ disease are more susceptible to calcium and vitamin D deficiency during the winter months. Deficiencies of these two nutrients are linked with a higher risk of tetany following surgery for Graves’ disease. Tetany is a condition of mineral imbalance in the body that results in severe muscle spasms. Mild tetany is characterized by tingling in the fingers, toes and lips. More severe forms can lead to death. Tetany occurs when the concentration of calcium in body fluids falls below normal. Low calcium levels can be caused by a lack of vitamin D. Fortunately, most forms of tetany can be successfully treated with adequate calcium and vitamin D.
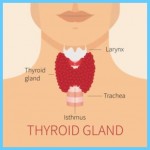
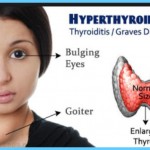
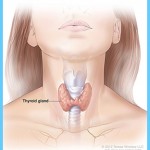
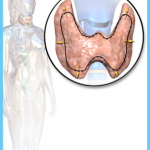
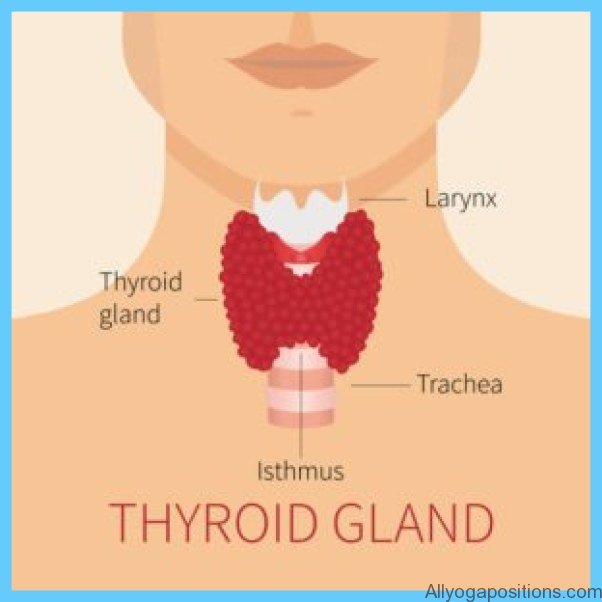
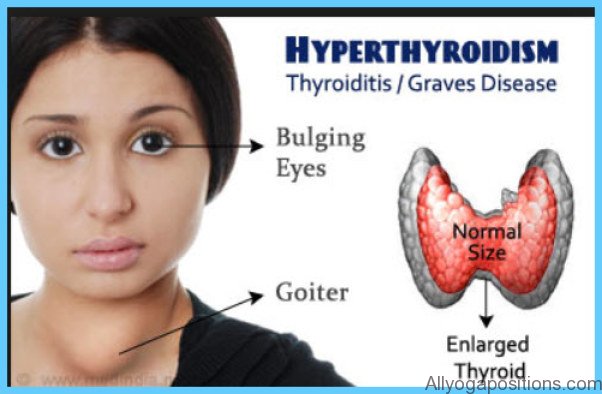
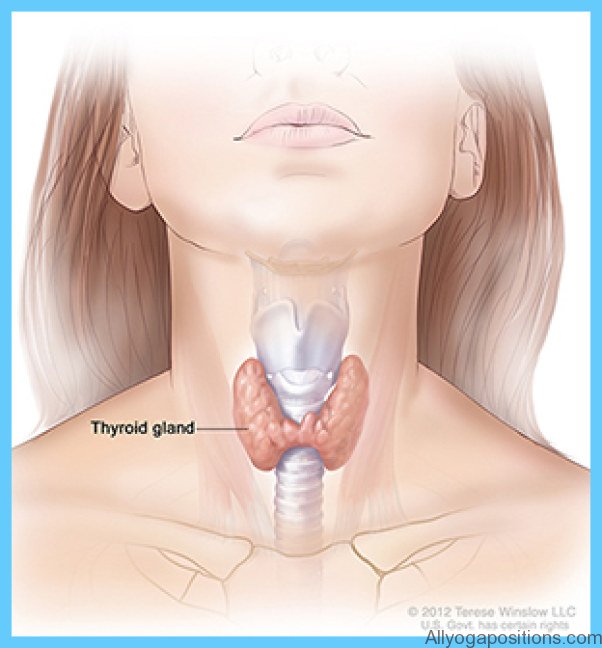
Calcium and Vitamin D Graves Hyperthyroidism Photo Gallery
To protect your bones and lower the risk of postoperative tetany, make sure you meet your daily requirements for each of these essential nutrients—see the RDA tables on pages 14 and 16 in chapter 1. Use the Calcium in Foods and Vitamin D in Foods tables there to help you boost your intake of these nutrients from foods. Unfortunately, there are only a few good food sources of vitamin D. We meet the majority of our vitamin D requirements by exposing our skin to sunlight during the summer months.
Calcium and Vitamin D Supplements
If you are not meeting your daily targets for calcium and vitamin D through your diet, I strongly recommend that you take a supplement. If you take a multivitamin and mineral supplement, it should have 400 IU of vitamin D in it (most brands do). But calcium is a large mineral and manufacturers can’t fit very much in a multivitamin and mineral pill. For this reason, you have to rely on a separate calcium supplement. Here are a few guidelines to help you choose among a multitude of products:
• If you consume at least three to four servings of dairy products or calcium-fortified beverages each day, you’re getting approximately 900 to 1200 milligrams of calcium. For every serving you’re missing and not making up with other calcium-rich foods, consider taking a 300 milligram calcium supplement.
• When choosing a supplement look at the source of calcium. Studies show that calcium citrate supplements are better absorbed than those made from calcium carbonate. This is an important consideration if you’re over 50 years old or
you take medication that blocks the production of stomach acid (calcium carbonate requires more stomach acid for its absorption).
• Check the ingredient list to see how much elemental calcium each pill gives you. This is what you base your daily dose on.
• Consider choosing a calcium supplement with ipriflavone, a synthetic isoflavone that’s been shown to enhance the bone-building potential of calcium and vitamin D. To learn more about ipriflavone, turn to page 173 in chapter 10, “Osteoporosis.”
• Choose a calcium formula with vitamin D and magnesium, two nutrients that work with calcium to keep bones healthy.
• Spread larger doses throughout the day. If you must take more than 500 milligrams from a supplement, split your dose over two or three meals.
• The daily safe upper limit is 2500 milligrams of calcium from food and supplements combined. Too much calcium may cause constipation, gas and kidney stones in people with a history of the disease.
The Bottom Line…
Leslie’s recommendations for managing thyroid disease
1. If you have hypothyroidism and you’re concerned about your body weight, or if you’ve gained excess weight after treatment for Graves’ disease, embark on a healthy eating and exercise program. Start by keeping a food diary for two weeks to pinpoint areas that need to be improved upon.
2. Don’t skimp on iodine. The best sources of iodine are iodized table salt (all salt in America is fortified with iodine), seafood, plants grown on iodine-rich soil and animal foods from animals that graze on iodine-rich soil. But don’t get too much iodine, as intakes greater than 600 micrograms per day may lead to hypothyroidism. To keep your iodine intake within reason, avoid eating large quantities of kelp, dulse or other sea vegetables on a daily basis.
Hypothyroidism
1. If your doctor has determined that you have high blood cholesterol levels, read chapter 11 to get all my nutrition strategies to bring it down.
2. Boost your intake of B vitamins, in particular folate, B6 and B12.
3. Be sure you’re getting enough selenium. The best food sources include seafood, meat, whole-wheat products, wheat bran, wheat germ, Brazil nuts, Swiss chard and garlic. If you take a supplement, don’t exceed 200 micrograms per day.
4. If you are taking single iron supplements for iron-deficiency anemia, do not take iron pills with your thyroid medication, since iron can reduce your body’s absorption of the drug. Take your iron pill two hours before or two hours after taking your medication.
Graves’ Disease
1. Boost your intake of dietary antioxidants including vitamins C, E and beta-carotene.
2. Get more calcium and vitamin D in your daily diet. You need 1000 to 1200 milligrams of calcium and 200 to 600 IU of vitamin D each day.