Migraine is one of the most common and misunderstood of all diseases. It has disabling effects on millions of people, yet it is very often misdiagnosed and has no definitive cure. Women are three times more likely to suffer from migraines than men—a factor that may be related to the hormonal changes that occur during the menstrual cycle.
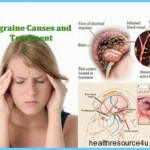
A migraine is a type of headache that results from inflammation of the blood vessels and nerves surrounding the brain. The exact causes of migraine headaches are not known, but they seem to be set off by changes in brain activity. Very often, specific substances, actions or stimuli in your body or environment may trigger migraines.
Although the symptoms, frequency and intensity of migraines vary widely, they are often acutely painful and incapacitating. Over 80 percent of migraine sufferers cope with some degree of headache-related disability. Treatment of migraines usually involves a two-pronged approach. Therapies focus on providing relief of symptoms and preventing or reducing future headache attacks.
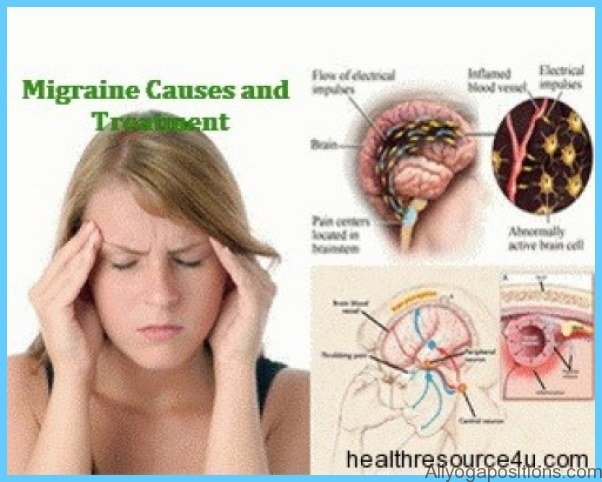
What Causes a Migraine?
People have been suffering from migraines for hundreds of years, but we still don’t clearly understand the underlying causes of this relentless disease. Research indicates that a migraine involves both the nerves around the brain and the blood vessels that feed the brain. Scientists have recorded a spreading pattern of electrical activity within the brains of people with migraines, which may be responsible for some of the classic migraine symptoms. Many people also experience a decrease in blood flow to various parts of the brain, again connected with the onset of migraine. More recently, there has been some evidence that serotonin, a powerful chemical that has the ability to constrict blood vessels, may help stimulate the migraine mechanism.
Symptoms
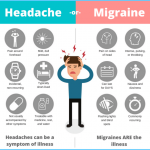
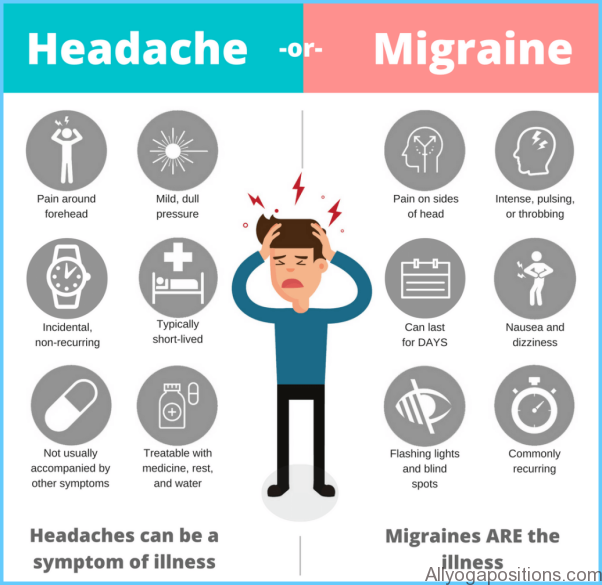
There are two common types of migraine and they each have slightly different symptoms:
1. Migraine with aura. This is referred to as a classic migraine. The aura is a set of neurological symptoms that occur approximately 10 to 30 minutes before the headache starts. During the aura phase, you may experience visual disturbances, such as flashing lights or geometric patterns in front of your eyes, or you may even suffer brief vision loss. It is not uncommon to feel dizzy and confused or to have some facial tingling and muscle weakness as the aura progresses. Migraines with auras affect only 10 to 20 percent of migraine sufferers.
2. Migraine without aura. This is known as a common migraine, and it affects many more people than the classic migraine. Although you will not have an aura, you may have mood swings, feel depressed and fatigued or lose your appetite just before the migraine strikes.
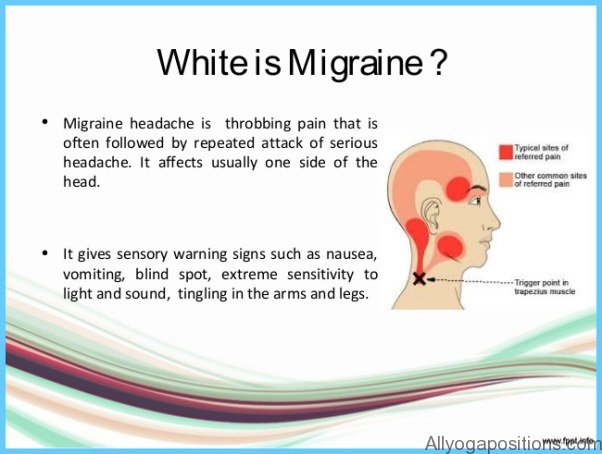
A pulsing, throbbing pain characterizes both types of migraine. The pain is often felt only on one side of your head or behind one eye, but it may spread to involve your entire head at a later stage. Migraines are usually aggravated by physical activity and are often accompanied by severe nausea and vomiting. They may also be associated with a wide variety of other symptoms, including heightened sensitivity to light, noise and odor, diarrhea, facial swelling, nasal congestion and scalp tenderness. Once the headache has subsided, it will usually leave you feeling extremely fatigued, listless and irritable.
Although there are some characteristic symptoms of a migraine, most migraines don’t conform to a typical pattern. You may be lucky and only suffer a migraine once in a while, or you may be incapacitated by attacks that occur as often as three times a week. The intensity of pain that you feel can vary from reasonably mild to completely debilitating. Migraines also vary in length from a brief, 15-minute episode to an attack that can last a week. On average, the duration of a migraine ranges between 2 and 72 hours.
Who’s at Risk?
Migraine is a universal condition that affects approximately 6 percent of men and 15 to 18 percent of women. Although migraines can strike children and adolescents, they most often affect women between 25 and 55 years of age. As many as 50 to 70 percent of all migraine sufferers have a family history of the disease, indicating that these headaches may be hereditary. However, a specific migraine gene has not yet been found.
Diagnosis
Because of the wide variation in symptoms, migraines are quite difficult to diagnose. They can often be confused with other types of headaches, such as tension or sinus headaches. To help doctors make an earlier diagnosis, the American Headache Society has recommended a detailed set of criteria for assessing migraine symptoms. It is reasonable to assume you suffer from migraines if your headaches have some of the following characteristics:
• a sequence of at least five attacks that last between 2 and 72 hours
• pain that is located on one side of your head, sometimes spreading to both sides
• pain that is pulsating or throbbing
• pain that prohibits or limits daily activity
• pain that is aggravated by physical activity
• nausea or vomiting during headache attacks
• sensitivity to light, noise or smell during headache attacks
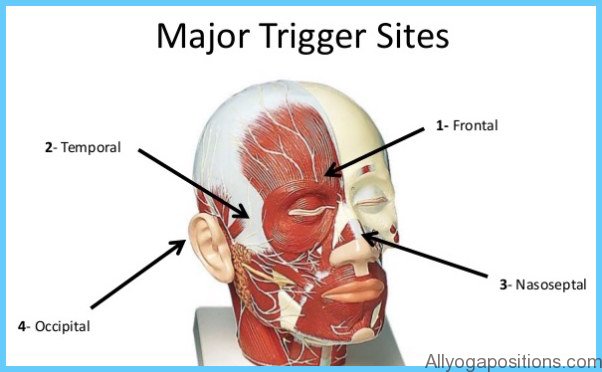
Migraine Triggers
In some cases, certain stimuli or triggers that you experience as part of your normal life provoke migraines. By avoiding these triggers, you may be able to reduce the frequency or severity of your attacks. Although triggers don’t actually cause a migraine, they do seem to influence the activities in your brain that stimulate the disease. Often, you will be sensitive to the combined effect of more than one trigger.
There are many common migraine triggers and you must determine which ones affect you. Keeping a migraine headache diary is a good way to identify the circumstances that set off your migraines.
1. Diet Certain foods and food additives are well-known migraine triggers. Alcoholic beverages (especially red wine), foods treated with MSG (monosodium glutamate), foods that contain tyramine (e.g., aged cheeses, soy sauce) or aspartame (NutraSweet™) and foods preserved with nitrates and nitrites all may provoke migraines. Chocolate, caffeine and dairy products are other known culprits.
2. Lifestyle Changes in your behavior or your surroundings can encourage migraines. If you alter your eating or sleeping habits, experience high levels of stress or smoke cigarettes, you may find yourself struggling with more frequent migraines.
3. Environment Some people find that bright lights or loud noises will bring on a migraine. Weather or temperature changes and physical exertion are common triggers, and even changing time zones may affect your headache frequency. Strong odors, perfume, high altitudes and computer screens are other recognized triggers.
4. Female hormones Women may be more susceptible to migraines because of the estrogen cycles associated with menstruation. Migraines become more prevalent in females after puberty, reaching a peak at age 40, and then declining in frequency as women age. But almost two-thirds of women who suffer from migraines will experience a worsening of their headaches during their period. Up to 15 percent of women will get migraines only during their period, as what is called true menstrual migraine. Menstrual migraines are typically without aura and last longer than other migraines. They are also more difficult to treat. To prevent these debilitating headaches, it is extremely important for women to avoid migraine triggers during the premenstrual week (you’ll find a list of dietary triggers later in the chapter).
5. Oral contraceptives and estrogen therapy also seem to make migraines worse. If you take these medications and suffer from migraines, you may want to speak to your doctor about being on a low-dose estrogen regimen.
6. Pregnancy Migraines are more common in early pregnancy but usually improve by the second trimester. In a small group of women, pregnancy migraines will worsen throughout their pregnancies. During pregnancy, women should pay special attention to avoiding dietary and environmental triggers, sticking to regular sleeping and eating schedules, getting regular exercise and managing stress (as should all women with migraines).