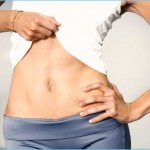
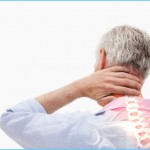
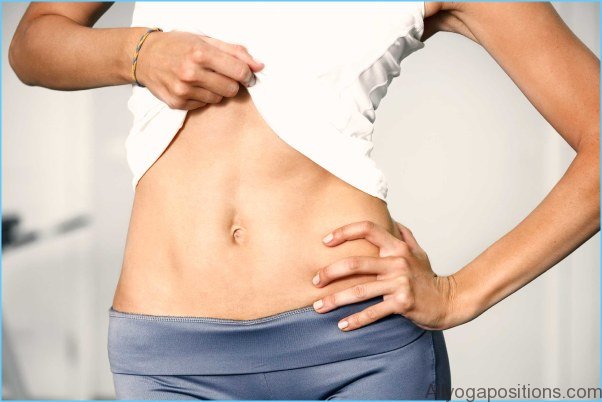
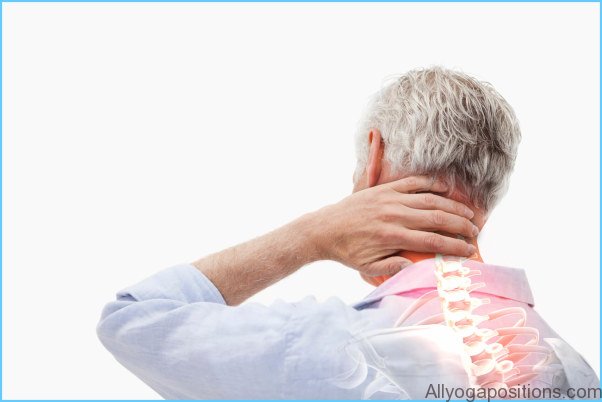
Your gut flora, the medications you take, and the food you eat all have the potential to inflame the “pain brain” and aggravate the “pain body.” So it makes sense to rethink what you are putting in your gut each day. Although my recommendations are quite simple and not hard to implement, they will help you make the positive changes you both want and deserve for your mind and body. And it won’t take long to see results: a change in eating habits can lead to changes in the gut’s flora (for better or for worse) in as little as 24 hours.
Opioid-Based Painkillers: Tough Choices
If you haven’t already begun taking potent opioid-based pain medications, my advice is to make a concerted effort to avoid them. The long-term effects on your health are negative, and they simply aren’t the answer to chronic pain. Ongoing research is focusing on ways to tweak these medications to make them more efficacious and less problematic, but we just aren’t there yet. And I have found that the less my patients focus on medications, the more successful they are at using alternative methods to control their pain and manage flare-ups.
Rethink What You Put in Your Gut Photo Gallery
However, if you are already on opioid-containing painkillers, you have some soul-searching to do. Letting go of them can be anxiety inducing, and you may wonder how you’ll be able to manage the pain without them Yet at the end of the day, you should ask yourself this question: “Do I plan on taking these medications for the rest of my life?” Before you answer, think about how your pain medications have changed your life, in both positive and negative ways. How effective have they been in helping you function and interact with the world? Which side effects have they caused, and are you prepared to live with them over the long haul? It will help to talk to your family, trusted friends, and doctors. They often see changes in you that you may not be aware of.
If you decide that you would like to get off of opioid painkillers, it’s important that you have a plan and as much support as possible. Here are some tips that can help:
• Consider enlisting the support of others, apart from your doctor, as you transition away from long-term opioid use. Those you may find helpful can include a counselor, life coach, therapist, acupuncturist (acupuncture helps with withdrawals), and/or a support group made up of those who have gone through a similar process.
• Consider the timing of your transition, taking into account things like family events and holidays. December is usually not a good month for making challenging life changes.
• Develop a plan, program, or philosophy regarding the management of your pain in the future. Giving up opioids with no Plan B probably won’t work in the long run. Write down how you intend to manage your physical and emotional health, and refer back to your notes during trying times.
• Consider a buprenorphine-containing medication regimen if withdrawal becomes too problematic. Buprenorphine binds tightly to the same receptors as the opioids, triggering partial activation and partial blocking. In many people, this is enough to prevent cravings for more medication.