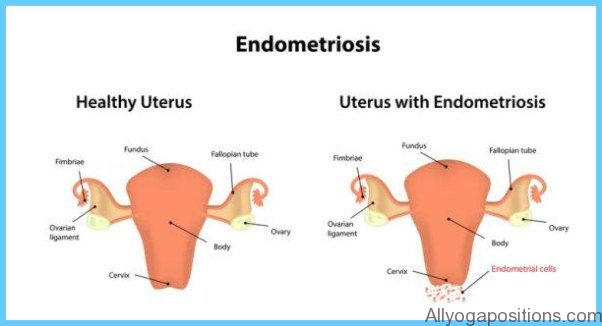
Endometriosis is a poorly understood disease that afflicts as many as one in ten women. The condition develops when uterine-type cells grow outside of the uterus. These cells may travel throughout the body and attach to a number of different areas. The misplaced cells develop into nodules, lesions, implants or growths that are affected by the hormonal fluctuations of the menstrual cycle. These growths cause pelvic pain, pain during intercourse, infertility and other problems. There’s no question that endometriosis can influence every aspect of a woman’s life—her ability to have children, to work and to relate with loved ones.
What Causes Endometriosis?
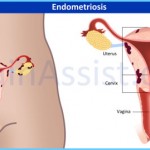
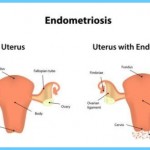
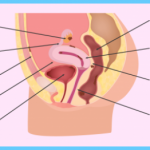
The uterus, a reproductive organ located within the abdominal cavity, is lined with a type of tissue called endometrium. When you have endometriosis, tissue that looks and acts like endometrium is found living outside of your uterus. In most cases, the misplaced tissue is discovered growing somewhere within the abdominal cavity. It may be found attached your ovaries, bowel, bladder, fallopian tubes or cervix. Although rare, the appearance of endometrial tissue in other sites around the body including the
What Is Endometriosis Symptoms Treatment Causes Photo Gallery
lung, arm and thigh, is possible. Endometrial growths can vary in size and penetration of the surrounding tissue. Rest assured that endometrial growths are generally not cancerous—they are normal types of tissue found growing outside the normal location.
During the course of a normal menstrual cycle, the endometrial lining of your uterus gradually builds up in preparation for pregnancy. If you don’t become pregnant, the lining breaks down, bleeds and is discharged from your body during your period. Unfortunately, the endometrial tissue living outside of your uterus responds to the hormonal cycles of menstruation in exactly the same way. But, unlike the menstrual flow from the uterus, the blood from the misplaced tissue has no place to go. This causes episodes of internal bleeding and inflammation that can result in internal scarring, severe pain and infertility.
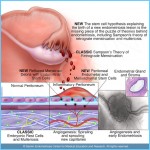
Scientists still don’t know what causes endometriosis. The most commonly held view is the retrograde menstruation theory. This theory suggests that menstrual tissue occasionally flows backwards through the fallopian tubes during menstruation. The tissue is discharged from the fallopian tubes into the abdomen, where it becomes implanted and develops into endometrial growths. Another theory proposes that endometrial tissue may be distributed from the uterus to other parts of the body through the lymph glands or blood vessels. In some cases, endometrial tissue may be accidentally transplanted into distant sites through surgical procedures. It’s possible that hereditary factors are involved making some families more susceptible to the disease. Eventually, scientists may discover that endometriosis is caused by a combination of factors.
Symptoms
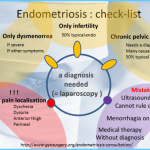
The most common symptom of endometriosis is pain before and during menstruation. Symptoms include
• severe menstrual cramps
• irregular vaginal bleeding
• pelvic pain
• painful sexual intercourse
• painful bowel movements
• pain during exercise
• painful and frequent urination
• backache
• constipation or diarrhea
• fatigue
The symptoms of endometriosis have little to do with the extent of the endometrial growths. Some women with mild endometriosis and small growths may experience excruciating pain, while other women with large growths and severe endometriosis may have no painful symptoms at all. Each case of endometriosis is unique. Symptoms usually start after the onset of menstruation and subside after menopause, when the growths tend to shrink or disappear.
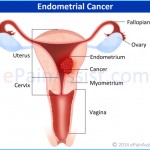
Infertility affects 30 to 40 percent of women with endometriosis. Severe endometriosis, which causes extensive scarring and organ damage, is considered one of the three major causes of infertility. While many women with endometriosis fear cancer, the condition is rarely associated with endometrial cancer—fewer than 1 percent of women with endometriosis go on to develop endometrial cancer.1
THE BOWEL
Many women with endometriosis experience on-going gastrointestinal discomfort, including diarrhea, painful bowel movements and general intestinal distress. In fact, the data registry of the Endometriosis Association (a U.S.-based nonprofit organization) reported that 79 percent of women with endometriosis experience these symptoms.2 Gastrointestinal symptoms were the most commonly reported symptoms, along with painful periods and fatigue.
Indeed, many of my clients with endometriosis complain of pain, nausea, feeling full, bloating and altered bowel habits. Occasionally women report vomiting. Studies have revealed that endometriosis is associated with changes to the intestinal tract, such as altered motility and bacterial overgrowth. There are four possible reasons why women with endometriosis experience bowel problems:
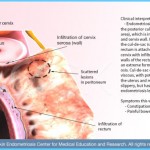
1. Endometrial growths develop directly on the bowel, usually the latter part of the
large intestine. This usually causes painful bowel movements, a sense of rectal pressure, urgency to defecate or bloody stools. Most specialists carefully check the
bowel for the presence of endometriosis but, because the intestine is so long, it is possible for growths to be missed. For the most effective treatment, many endometriosis experts recommend surgically removing the portion of bowel affected.
2. Adhesions can result from the endometriosis itself, or from past surgeries. Adhesions are fibrous bands or structures by which parts abnormally adhere. These adhesions pull on the bowel and cause pain.
3. prostaglandins may cause intestinal symptoms—such as diarrhea, nausea and vomiting—in women who do not have any evidence of endometriosis on their bowels. During a woman’s period, these symptoms can be caused by prostaglandins, compounds produced by the body that control the smooth muscle of the uterus, bowel and blood vessels.
4. Symptoms may be caused by an overgrowth of Candida albicans (candidiasis), a fungus responsible for causing yeast infections in women. In this case, intestinal symptoms often include constipation and/or diarrhea, stomach pain, gas, bloating and rectal itching. Women with this yeast infection often develop food sensitivities, which can contribute to gastrointestinal upset. Usually treatment of the candidiasis provides women relief of these symptoms. Unfortunately, diagnosis of yeast overgrowth is not easy to obtain, as this condition is new and controversial among the medical community.
Women with endometriosis are often told by their doctor that they have irritable bowel syndrome (IBS). Unfortunately this diagnosis is not very helpful because it does not indicate what the underlying problem is. IBS is really just an umbrella term used to describe gastrointestinal distress when no other diagnosis can be made. During IBS, the muscular contractions of the bowel become uncoordinated, resulting in alternating constipation and diarrhea, gas, bloating and nausea. These symptoms can be caused by any of the four reasons listed above. Having your doctor thoroughly investigate the cause of your bowel problems is important for effective treatment.
Who’s at Risk?
More than 5.5 million North American women and girls have endometriosis. The disease occurs most often in women of childbearing age, affecting 10 to 15 percent of women between the ages of 25 and 44, but teenagers can also suffer from endometriosis.
The disease is believed to run in families, so you are more at risk if you have a first-degree relative (e.g., mother, sister) with endometriosis. Other risk factors include being of Caucasian descent, having your first child after the age of 30 and having an abnormal uterus.
Diagnosis
If you are suffering from the symptoms listed above, or you are having difficulty becoming pregnant, your doctor may suspect that you have endometriosis. He or she will evaluate your medical history and conduct a complete physical examination, including a pelvic exam. It is sometimes possible to actually feel an endometrial growth during the pelvic exam.
Most often, an accurate diagnosis can be made only if patches of endometrial tissue can be seen. To determine the presence of misplaced tissue, your doctor will conduct a minor surgical procedure called a laparoscopy. A small surgical tube with a light attached is inserted through a small incision in your abdomen. This allows your doctor to examine your abdominal organs and to evaluate the size and extent of any endometrial growths. In some cases, tissue samples may be removed and sent to a laboratory for microscopic examination.